Gabapentin Abuse and Treatment in Orange County, CA
What is Gabapentin?
In 2004, it was also approved for use as an analgesic (pain reliever) for post-herpetic neuralgia, which is a painful condition that affects the skin and nerves of people who have had shingles. According to the Drug Enforcement Administration (DEA), the number of gabapentin prescriptions doubled between 2009 and 2017.
Because it’s thought to have a low risk of abuse, it has a long list of off-label uses, meaning that doctors will prescribe it for issues other than those for which the FDA has approved it.
These include:
It is estimated that 83% to 95% of all gabapentin use is off-label, which accounts for approximately 90% of sales. This is because Pfizer, the pharmaceutical company that originally marketed gabapentin, promoted its off-label use, which is an illegal marketing tactic. Pfizer was fined $420 million as a punishment for their illegal marketing.
How is Gabapentin Used?
Gabapentin must be taken regularly and at the same time every day to keep the level of gabapentin in the body stabilized. Not taking it at the same time could increase seizures and other symptoms for which it has been prescribed.
Be Brave. Get Help.
Common Questions
Gabapentin is the name of the ingredient. Neurontin, Gralise, Gabarone, and Fanatrex are brand-name medications made of gabapentin.
Although it isn’t widely known and is less popular as a street drug than other medications, when it is used on the street it is typically called “gabbies” or “johnnies.”
It’s part of a category of drugs known as anticonvulsants, antiepileptic drugs, or anti-seizure drugs. As implied by the name, these types of drugs are typically prescribed for epilepsy and seizures; however, they have other uses and are often prescribed for other issues as well.
Reach out to verify your insurance coverage for addiction treatment
How Many Prescriptions for Gabapentin are Written Every Year in the US?
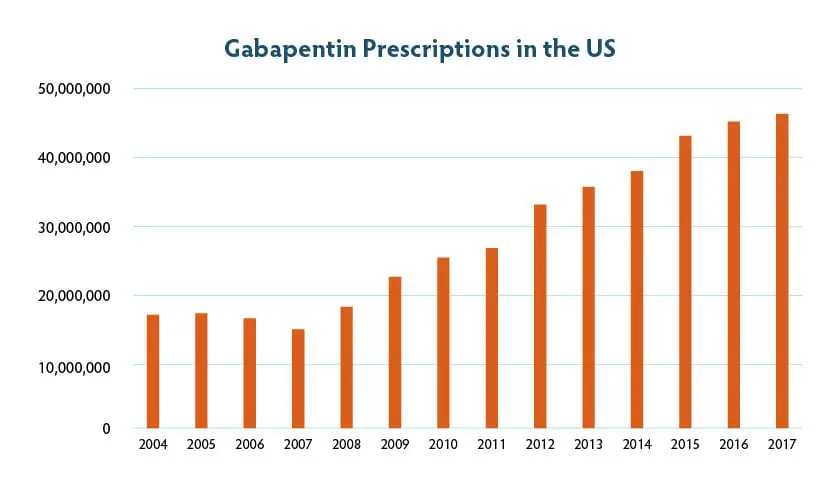
As is clear from the statistics reported, the number of prescriptions has increased significantly over the past decade. This is due to the increasing number of prescriptions that are off-label as well as the illegal marketing of off-label uses to the public.
What Precautions Should Be Taken Before Using Gabapentin?
- Are allergic to gabapentin
- Have any other allergies
- Have a history of kidney disease
- Have a mental health disorder
- Abuse drugs or alcohol
- Have breathing problems
- Are taking antacids that contain aluminum or magnesium, as these may interfere with the absorption of gabapentin
- Are taking any other medications that may cause drowsiness, such as:
- opioids
- cough suppressants
- alcohol
- marijuana
- sedatives
- anti-anxiety medications
- muscle relaxants
- antihistamines
Where is Gabapentin on the Schedule of Controlled Substances?
That being said, some states have opted to place gabapentin on the schedule, categorizing it as a Schedule IV or V substance. This classification means that it poses a low risk of misuse and abuse; however, these states believe that it poses enough risk to be placed on the schedule.
For reference, Schedule I drugs pose the highest risk of addiction and serve no medical purpose, whereas Schedule V drugs pose almost no risk of addiction and abuse.
As of 2019, the following states have reclassified gabapentin as a controlled substance: Kentucky, Michigan, West Virginia, and Tennessee. Additionally, pregabalin, a substance very similar to gabapentin, is a Schedule V drug under the Controlled Substances Act.
Effects and Overdose
Side Effects
Although gabapentin is safe to take, patients might experience some of the following side effects when taking gabapentin, particularly over the long term.
These effects may include the following:
- Anxiety
- Blurred vision
- Diarrhea
- Dry mouth
- Fever
- Headache
- Increased appetite
- Loss of coordination
- Nausea/vomiting
- Runny nose
- Uncontrollable shaking
- Weight gain
- Back pain
- Constipation
- Dizziness
- Ear pain
- Flu-like symptoms
- Heartburn
- Joint pain
- Memory issues
- Red/itchy eyes
- Swollen hands, feet, and ankles
- Unwanted eye movements
- Weakness
Long-term Effects
Is it Possible to Overdose on Gabapentin?
Can Gabapentin Be Abused?
Gabapentin is not a substance that is tested for during treatment, so people will use it to try to get high in the absence of other drugs. The Drug Abuse Warning Network reported that about 20% of patients who are in methadone maintenance treatment misuse or abuse gabapentin. Gabapentin also tends to be abused because it is relatively cheap and widely available.
It’s also frequently abused along with muscle relaxants, opioids, or anxiety medications, all of which can produce a “high” or euphoria, making it important for some people to take an anxiety test to understand their emotional health.
A study on gabapentin abuse showed that, out of a group of people found to be using it without a prescription, 56% of people took it with an opioid and 27% of people took it with a muscle relaxant, or anxiety medication. Mixing gabapentin with alcohol or other drugs can make people tired or dizzy, or can increase side effects. Between 2008 and 2015, the Drug Abuse Warning Network reported that emergency room visits related to gabapentin increased by 90%.
How Can a Person Stop Using Gabapentin Safely?
What are the Signs of Gabapentin Abuse?
- Taking a higher dosage than prescribed
- Taking it more frequently than prescribed
- Using it without a prescription
- Buying it on the streets
- Stealing or taking pills from others
- Isolating oneself from friends and family
- Using it together with other drugs
- Irregular sleep patterns/habits
- Failing to keep up with life, school, and work responsibilities
- Spending increasing amounts of money to obtain it
- Refusing to stop using gabapentin
- Lying about drug use
- Uncontrollable shaking
- Poor coordination
- Difficulty speaking
- Memory loss
- Depression
- Anxiety
What Are the Withdrawal Symptoms of Stopping Gabapentin Use?
Because withdrawal symptoms can be quite serious and even life-threatening, it is best to stop using a drug through a medically supervised detox. If a medically supervised detox is not available, it is best to taper off of the drug slowly so that the body has time to adjust to a smaller dose of the substance. Gabapentin withdrawal typically begins between 12 hours and 7 days after the last dose.
Symptoms of withdrawal include:
- Insomnia
- Anxiety
- Sweating
- Pain
- Gastrointestinal symptoms
- Tremors
- Increased heart rate
- High blood pressure
It is also important to note that withdrawal symptoms are more likely to occur if patients have been taking gabapentin along with other substances. People who experience any confusion or psychosis after stopping substance use should seek medical help immediately.
Treatment Options for Gabapentin Abuse in Orange County, CA
Treatment options will then depend on whether the person has taken other drugs with gabapentin and might need to treat opioid addiction or some other concurrent disorder. Patients shouldn’t be afraid to consult their doctors and ask for referrals to other healthcare professionals to be able to create comprehensive and individualized treatment plans.
Need to Understand the Issues Underlying Substance Abuse
Therapies
Behavioral therapies include individual therapy, group therapy, and family therapy. One example is cognitive-behavioral therapy, which can occur either on a one-to-one basis with a psychotherapist or in a group setting. Cognitive-behavioral therapy focuses on thought patterns and behaviors surrounding drug use, and on ways in which patients can adapt their thinking and behavior to support recovery.
Another group therapy option is Narcotics Anonymous, which is based on the principles of Alcoholics Anonymous and revolves around the peer support of people going through the same process. This might be a good option for people struggling with multiple substances. It is always helpful to have the support of friends and family as well, as addiction treatment can be difficult to succeed without any support.






